Suspected Salmonellosis in Horses: What Do You Do?
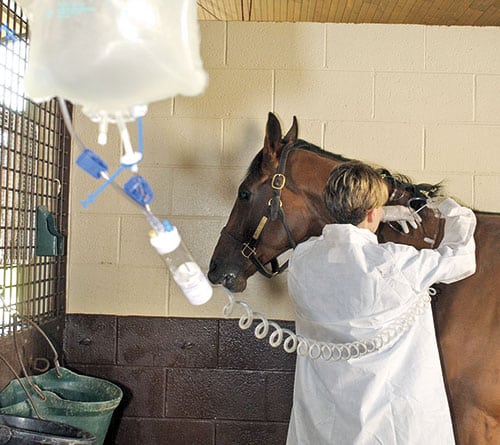
Learn to navigate the murky waters of diagnostic testing for this zoonotic disease
Watery, projectile fluid coming from the back end of an adult horse is hard to miss, but the underlying cause often isn’t easy to see. In approximately 50% of all cases of adult diarrhea (caused by enteritis/colitis—inflammation of the small intestine and colon, respectively), veterinarians never identify a definitive cause, even if an infectious disease is likely to blame, and even with thorough diagnostic testing.
“When diagnosable, Salmonella is a frequently fingered cause of diarrhea in adult horses, and Salmonella Typhimurium is a common serotype isolated,” says Luis (Memo) Arroyo, Lic. Med. Vet., DVSc, PhD, Dipl. ACVIM, an associate professor at the University of Guelph’s Ontario Veterinary College, in Canada. “Arriving at a final diagnosis remains a cornerstone at referral hospitals and does help with infectious control and biosecurity protocols for field practitioners, owners, and farm personnel/managers.”
Due to Salmonella’s zoonotic (transmissible between animals and humans) potential, testing is especially important in outbreak situations or cases where the bacterial disease is suspected.
In this article, we’ll describe the tests available to veterinarians during their diagnostic work-up, limitations associated with interpreting those results, and information on treating and controlling this highly infectious condition.
Diagnostic Options for Salmonella spp
When working up a case of diarrhea in an adult horse, veterinary practitioners can choose from several tests. One option, which is the equivalent of throwing a net out to catch fish, is an “enteric panel” from a commercial laboratory. The advantages of this approach include:
- Cost. A panel is more economical than ordering a slew of individual tests.
- Screening for multiple infectious agents. Salmonella spp and Clostridium spp (perfringens and difficile) are the most common infectious causes of colitis in adult horses, but veterinarians must also rule out Potomac horse fever (PHF, caused by Neorickettsia risticii bacteria) and equine coronavirus. Other, less common causes of colitis include Lawsonia intracellularis, rotavirus, and Rhodococcus equi.
If practitioners suspect salmonellosis, it is possible (and reasonable) to test specifically for its causative pathogen. “Several tests are available for Salmonella testing, but a DNA-based test (polymerase chain reaction, or PCR) or a bacterial culture with microbial susceptibility that can help them select an appropriate antibiotic for treatment are the preferred tests in clinical cases,” says Arroyo.
According to a review article in Veterinary Clinics of North America: Equine Edition (Shaw and Stämpfli, 2018), PCR is a potentially highly sensitive and specific test with a fast turnaround. Culturing is slower but can provide more detailed information on the bacterial isolates as well as susceptibility. Knowing the exact serovar of Salmonella spp and its microbial sensitivity profile can benefit not only the patient but also the owners and handlers in terms of controlling disease spread between humans and animals alike.
Salmonella
This Gram-negative, rod-shaped, facultative anaerobic (can survive with or without oxygen), intracellular bacterium can affect an array of animals, including horses and humans. The species of concern is Salmonella enterica, which has several hundred antigenically distinct serovars. Of those, researchers consider subspecies enterica serovar Typhimurium the most important in equine practice.
—Stacey Oke, DVM, MSc
What To Do With the Test Results
Regardless of which test you choose, the result will be either positive or negative. However, that information still might not confirm whether a horse is infected with Salmonella spp.
A negative test
Negative results from the tests described can be frustrating for both clinicians and owners. However, even negative results can have a positive impact on managing diarrheic horses.
For example, a negative could mean the horse is not suffering from an infectious cause of diarrhea. Therefore, disease spread and zoonotic potential become less important. In such cases veterinarians should then look for other factors that contribute to gastrointestinal disease, including management (e.g., diet, exercise, travel), intestinal parasites, and noninfectious conditions such as inflammatory bowel disease and neoplasia (tumors).
Alternatively, negative results could reflect improper/inadequate laboratory technique or point to an emerging pathogen for which there is no good test.
Finally, false negatives can occur. For salmonellosis, a single bacterial culture or PCR test for detecting Salmonella spp might result in false negatives because animals shed Salmonella intermittently.
“Culture of several fecal samples collected over a period of three to five days is required to reliably identify intermittently shedding horses,” says Arroyo.
A positive test
If you think a positive test for Salmonella spp will end your diagnostic woes, think again. While veterinary medicine has benefited immensely from the widespread institution of PCR testing, it’s still not perfect. In the case of salmonellosis, PCR is sensitive (i.e., produces few false negatives) but does not indicate the presence of viable organisms—hence the phrase, “detection not infection.”
In other words, a positive test result still doesn’t support causation. The observed illness and colitis could be due to other infectious or noninfectious causes.
In addition, the test results might reveal more than one pathogen, leaving you unsure as to which one is the true culprit. For example, Kopper et al. (2021) identified multiple infectious agents per horse upon testing many animals with colitis. In that study the research team submitted 3,753 enteric disease fecal real-time PCR panels to IDEXX and 239 blood and fecal samples to Michigan State University’s Veterinary Diagnostic Laboratory (MSUVDL). Of those, one or more “potential enteric pathogens” (infectious agents capable of causing enteritis) were identified in 31.3% of submissions to IDEXX and 60.7% to MSUVDL.
These results show that simply identifying a pathogenic organism does not mean it’s the causative agent. Kopper et al. also demonstrated that testing results can vary depending on which laboratory you use.
Another complicating factor is even apparently healthy horses shed Salmonella. “Salmonella spp can be isolated from the feces and intestine in clinically normal horses and, therefore, detection of this microorganism from horses with no clinical signs … does not confirm a diagnosis of salmonellosis,” says Arroyo.
Presumptive Diagnosis of Salmonella: Now What?
Salmonellosis in horses ranges in presentation from an inapparent carrier state to pyrexia (fever), anorexia, and depression even without diarrhea or, in the worst cases, acute severe enterocolitis. Veterinarians must initiate prompt treatment—even before test results arrive. Without aggressive treatment, diarrhea of any cause can quickly result in dehydration, electrolyte and acid-based abnormalities, a protein-losing enteropathy (damage to the small intestine), and laminitis.
Prevent laminitis with cryotherapy
In their retrospective study Luethy et al. (2020) reported that laminitis occurred in 17 of 85 (20%) horses diagnosed with colitis from 2011 to 2019 at the University of Pennsylvania New Bolton Center’s D. Widener Hospital for Large Animals, in Kennett Square. Those horses tested positive for either Salmonella enterica (20), PHF (26), or equine coronavirus (16). The horses did not test positive for more than one infectious agent, and 23 (27%) horses had an unknown cause of colitis. Laminitis occurred in 15% of horses diagnosed with salmonellosis. Survival to discharge was 70% for horses with salmonellosis.
In that study the veterinary team initiated aggressive treatment, which might have resulted in the positive outcome (i.e., few laminitis cases and good survival to discharge). Therapies included intravenous fluids, flunixin meglumine (a non-steroidal anti-inflammatory drug), polymyxin B (an antibiotic that can also bind endotoxin), intragastric administration of an equine health product made from natural clay (di-tri-octahedral smectite, aka Bio-Sponge), and lower limb cryotherapy (cold therapy).
“Digital cryotherapy in horses with colitis reduces the incidence of laminitis from 33% in horses not treated with cryotherapy to 10% in horses treated with cryotherapy,” the authors stated. “Importantly, cryotherapy has been most effective at prevention of laminitis, not necessarily treatment of laminitis.”
Consider antibiotic use carefully
“Antimicrobial use in colitis cases is generally avoided unless signs of systemic infection are present,” says Arroyo.
Shaw and Stämpfli also warned vets of the dangers of administering antimicrobials to horses suspected of having salmonellosis. Nonetheless, Luethy et al. administered antibiotics to 60 of 85 (70%) study horses. All horses diagnosed with or suspected of having PHF received oxytetracycline, the preferred treatment for this cause of colitis. Fifty percent of the horses not diagnosed with PHF also received an antibiotic.
“Antimicrobial therapy may be warranted in acute diarrhea cases demonstrating severe neutropenia (abnormally low white blood cell numbers),” wrote Shaw and Stämpfli. “Antimicrobial drug selection should be based on culture and susceptibility patterns of the causative agents whenever possible. However, in cases of acute undifferentiated diarrhea in horses, antibiotics may be contraindicated because of further disruption of the microbiota. Furthermore, increased shedding of Salmonella was associated with administration of antimicrobials, and multidrug resistance in Salmonella spp is an emerging threat. Therefore, judicious use of systemic antimicrobials is strongly recommended.”
A group of Chilean veterinary researchers collected 545 samples from various environmental locations, surfaces, and patients within an equine hospital. Their goal was to determine the types of Salmonella within the hospital and their antimicrobial susceptibility. They obtained only 22 Salmonella isolates from samples collected in offices, the pharmacy, stalls, the surgery suite, on waterers, and other surfaces. Nineteen of those samples (86%) were resistant to at least one class of antimicrobials. Nine samples showed multidrug resistance, with resistance to up to eight antimicrobials.
“Ampicillin, chloramphenicol, streptomycin, sulfonamides, and tetracyclines seem to be the antibiotics with the most resistance issues for Salmonella,” says Arroyo.
In light of the demonstrated environmental presence of multidrug-resistant Salmonella isolates, these study results “highlight the importance of improving biosecurity programs to prevent disease in horses and the hospital personnel,” the authors stated.
Dr. Luis Arroyo
Containing disease spread
Salmonella spp are hardy and ubiquitous in the horse’s environment. “These bacteria can survive in the environment for months to years, depending on the serotype, humidity, and temperature,” says Arroyo. “And, even in freezing conditions, these resilient microbes remain viable and infective for weeks to months.”
Salmonella spp spread via the fecal-oral route, meaning infected horses contaminate feed and water sources with their fecal material. Again, inapparent carriers can shed Salmonella spp, similar to what happens with equine herpesvirus. The horse appears outwardly healthy yet still spreads bacteria. In a 2022 article Arroyo et al. estimated 0.8% of so-called “normal” horses in the general equine population showed evidence of Salmonella spp fecal shedding.
In cases of acute diarrhea or positive test results for Salmonella spp, veterinarians and handlers must practice strict biosecurity measures.
“Not only can Salmonella be spread in feces by asymptomatic horses to other horses, but humans as well,” says Arroyo. “Therefore, on even a single-horse farm, biosecurity measures should be implemented due to the potential zoonotic risk of Salmonella. I recommend adopting biosecurity measures at the farm level, and I am certain that this is taken seriously in everyday practice.”
Arroyo also recommends isolating positive horses for at least 30 days before retesting. At that time veterinarians should test five separate fecal samples 12 hours apart.
“Only if all of those tests are negative should the horse be permitted to leave isolation,” Arroyo says.
Containing Salmonella spp in the face of profuse, watery diarrhea can be challenging, but the same basic principles apply to salmonellosis as any other infectious diseases. Reduce environmental contamination by cleaning and disinfecting with appropriate agents, and ensure personnel are cognizant of their potential role in disease transmission. You can get detailed information on infectious disease control from the American Association of Equine Practitioners: aaep.org/guidelines/infectious-disease-control.
Take-Home Message
A negative test doesn’t always rule out an infectious component. Instead, wrote Kopper et al., a negative result “supports the concept that enteric disease in individual horses is multifactorial, and finding a definitive etiological cause can be elusive.”
Nonetheless, vets should pursue diagnostic testing because salmonellosis is an infectious disease that could result in outbreaks, both among horses and the humans handling them.

Written by:
Stacey Oke, DVM, MSc
Related Articles
Stay on top of the most recent Horse Health news with















