Managing Horse Wounds Without Antibiotics
As concerns over antibiotic resistance grow, equine veterinarians look for ways to treat wounds without reaching for these powerful drugs. Here are some of their options.
Share
ADVERTISEMENT
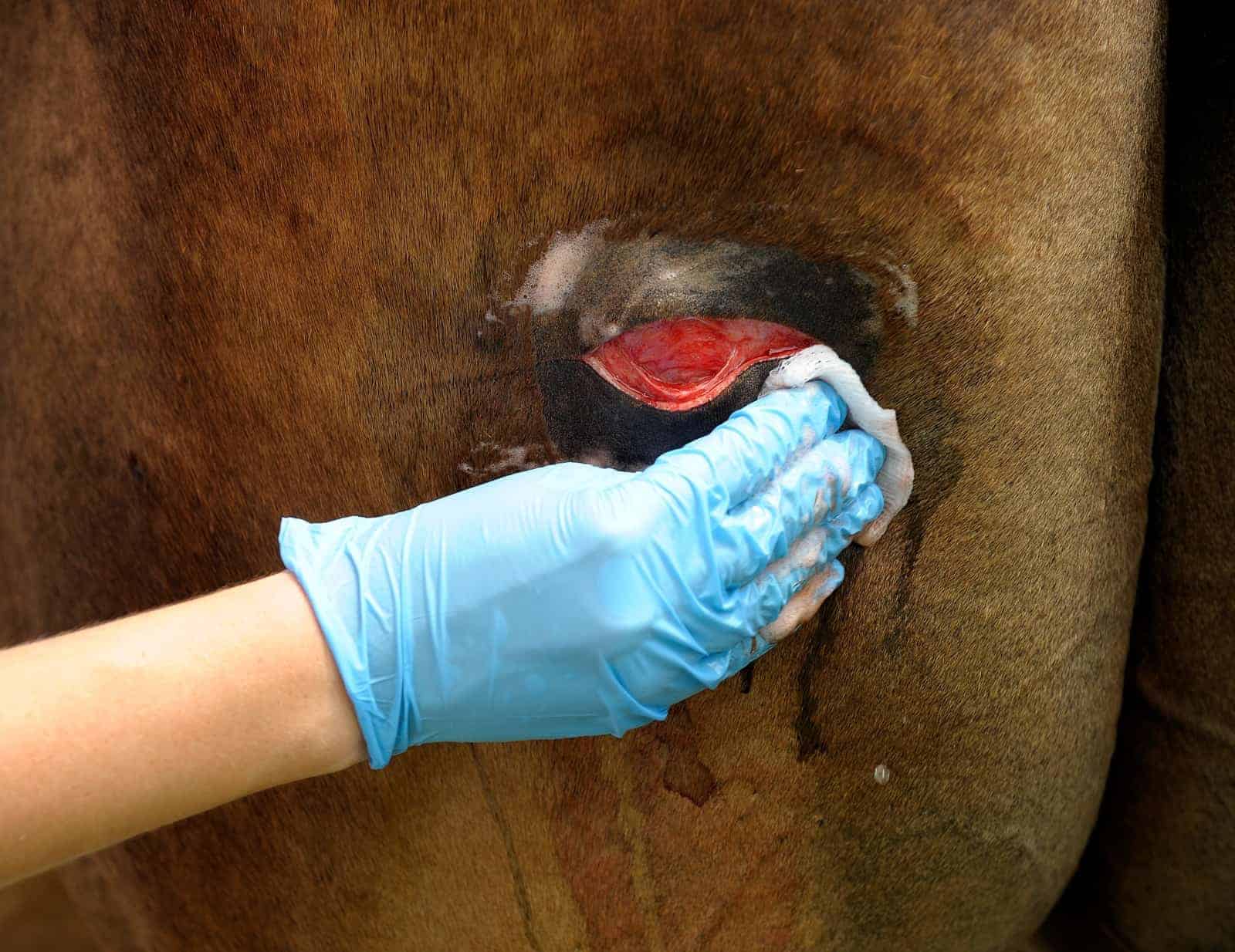
As concerns over antibiotic resistance grow, equine veterinarians look for ways to treat wounds without reaching for these powerful drugs. | Photo: Anne M. Eberhardt/The Horse
Debridement
The best way to deal with bacteria is to get rid of them, said Hendrickson, a professor in the Clinical Sciences Department at Colorado State University’s Veterinary Teaching Hospital, in Fort Collins.
“We have a tendency in veterinary medicine to want to kill the bacteria in situ, but I’m going to encourage you to remove them and throw them away and don’t let the patient have to deal with them at all,” he advised the audience
Create a free account with TheHorse.com to view this content.
TheHorse.com is home to thousands of free articles about horse health care. In order to access some of our exclusive free content, you must be signed into TheHorse.com.
Start your free account today!
Already have an account?
and continue reading.
Share

Written by:
Alexandra Beckstett
Alexandra Beckstett, a native of Houston, Texas, is a lifelong horse owner who has shown successfully on the national hunter/jumper circuit and dabbled in hunter breeding. After graduating from Duke University, she joined Blood-Horse Publications as assistant editor of its book division, Eclipse Press, before joining The Horse. She was the managing editor of The Horse for nearly 14 years and is now editorial director of EquiManagement and My New Horse, sister publications of The Horse.
Related Articles
Stay on top of the most recent Horse Health news with















