Regenerative Therapies: Helping Horses Self-Heal
The art (and existing science) of regenerative medicine in equine practice, and what’s to come
Regenerative therapy is an umbrella term encompassing any method that encourages the body to self- heal. Because it is drawing on its own properties, healing tissue more closely resembles native tissue than weak, disorganized scar tissue typically seen post-injury.
“The goal is to allow restoration of normal function and structure of the injured tissue to allow horses to perform at their previous level, whatever that might be, with a reduced risk of reinjury,” says Kyla Ortved, DVM, PhD, Dipl. ACVS, ACVSMR, assistant professor of large animal surgery at the University of Pennsylvania’s New Bolton Center, in Kennett Square.
She says the three main components of regenerative medicine that help tissues self-heal include:
- A scaffold upon which tissues can regenerate;
- Cells of the specific tissue type in need of repair or cells that help direct repair through signaling; and
- Bioactive signals/inflammatory mediators that direct the flow of traffic during the repair
“A specific therapy may incorporate some or all three of these components,” says Ortved.
Due to the regenerative therapy industry’s popularity and continued growth, many articles we’ve published review recent laboratory studies about stem cell production and data on efficacy and safety (you can find them at TheHorse.com/topics/regenerative-medicine). Here, we’ll review the basics of three regenerative modalities commonly used in equine medicine and when veterinarians and horse owners might consider each.
Types of Regenerative Therapies
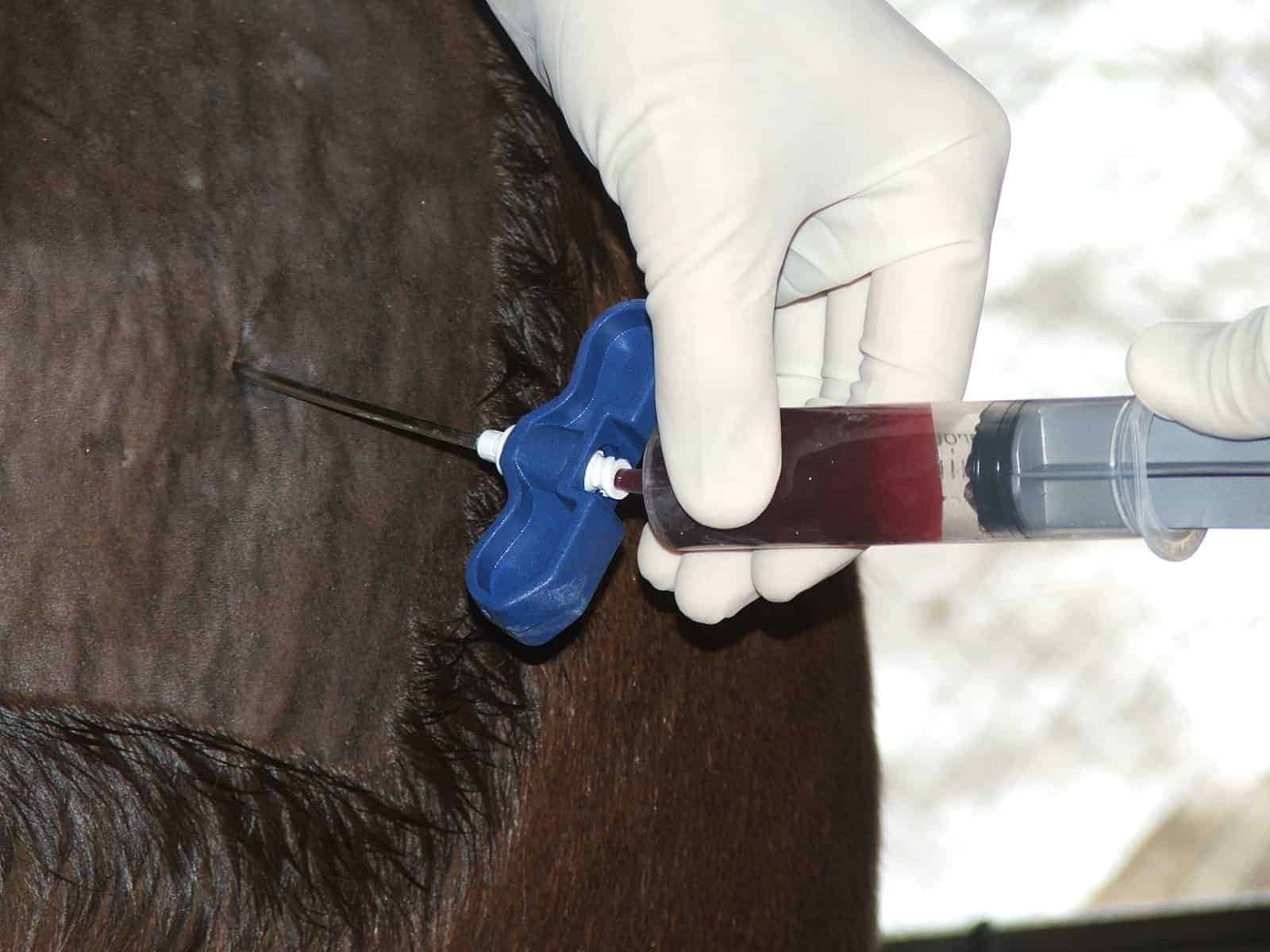
Platelet-rich plasma (PRP)
With this approach the practitioner collects blood from a horse and processes it using a commercial system that concentrates the platelets. When he or she injects that concentrated platelet product back into the horse, granules within the platelets release an array of growth factors that aim to facilitate and modulate the healing process. Specifically, granule-derived growth factors encourage target tissue cells at the injury site to migrate and proliferate, improve extracellular matrix synthesis, and stimulate blood vessel development.
Recently, “leukocyte-reduced” PRP has become many equine veterinarians’ PRP product of choice. These preparations contain fewer white blood cells (leukocytes) and, reportedly, inflammatory mediators than normal PRP products do. These mediators break tissues down, effectively counteracting the anabolic (tissue-building) effects of the platelets and their granules.
Autologous conditioned serum (ACS)
Veterinarians can easily prepare ACS by collecting a blood sample from the patient, then incubating it with special commercially available glass beads to stimulate interleukin-1 receptor antagonist protein (IRAP) production. They then inject the resultant IRAP-rich serum sample back into the patient at the target location or injury site. This protein blocks the action of interleukin-1, a powerful and damaging pro-inflammatory mediator. Additionally, glass bead incubation stimulates the production of anti-inflammatory mediators and growth factors similar to those found in PRP.
Ortved says it’s important to remember that all biologics, including PRP and IRAP, contain various concentrations of growth factors and bioactive protein.
“Remember, they are made from your horses’ blood and, therefore, contain all of the components in blood, just in varying concentrations,” she says.
Regenerative therapies that contain high concentrations of IRAP include IRAP II, autologous protein solution (APS), and bone marrow aspirate concentrate (BMAC).
Stem cell therapy (SCT)
In certain tissues, such as adipose (fat) and bone marrow, we can find specific cells that have the ability to self-renew and grow more than 200 types of body cells. Veterinarians can isolate these cells, called stem cells or progenitor cells, and either:
- Immediately concentrate and inject them directly back into the same horse at the target location, or
- Culture them in a lab to multiply before injecting them back into the
Perhaps more important than their ability to differentiate into other cell types, stem cells have “powerful anti-inflammatory properties and play a central role in coordinating healing in all types of tissues through cell-to-cell signaling,” Ortved says.
Which of these three modality types will provide the most benefit to your horse depends on a variety of factors that you and your veterinarian will consider.
Choosing an Implement
In a study published in June 2018, surveyed horse owners listed PRP and IRAP as two of the 10 most popular equine rehabilitation modalities available. Some said they also used stem cell therapy, but not as frequently as PRP and IRAP.
“I think the main reason that stem cell use has been dipping in the U.S. is because consistent efficacy has yet to be achieved,” says Ashlee Watts, DVM, Dipl. ACVS, equine orthopedic surgeon and director of Texas A&M University’s Equine Orthopedics and Regenerative Medicine Lab, in College Station. She says that in some horses stem cells appear to be highly effective. “In others, it’s as if we had done nothing in addition to routine therapy and care,” she adds. “We think this is because some of the methods used to prepare stem cells was rendering them ineffective in most horses.”
Lisa Fortier, DVM, PhD, Dipl. ACVS, James Law professor of equine surgery at Cornell University and a clinician at Cornell Ruffian Equine Specialists, in Ithaca, New York, concurs: “The variability in the product we are delivering … presently applies to all regenerative therapies: PRP, IRAP, APS, and stem cell products alike.”
Putting aside the conundrum of product optimization for the moment, let’s look at when and how practitioners are using these therapies in horses.

Musculoskeletal Injuries
Tendon, ligament, and joint injuries are among regenerative medicine’s most frequent targets. This is partly because musculoskeletal conditions can limit a horse’s functionality.
Take, for example, a superficial digital flexor tendon (that runs down the back of the leg from just above the knee or hock to the pastern) core lesion presumably caused by overloading the tissue. This is the most common cause of tendon and ligament injuries in athletic horses, and no one treatment approach has resulted in fast and durable repairs. These injuries typically require months of rest, rehab, and careful return to work—a frustrating and economically draining process that often fails due to the high rate of reinjury.
Because, again, regenerative medicine involves products that mitigate inflammation and stimulate normal, healthy tissue production instead of laying down weak scar tissue prone to future injury, our sources often reach for them when managing soft tissue and joint injuries.
“For tendons, I start with PRP while culturing the horse’s own stem cells, which can take several weeks,” Fortier says. “This way, we are addressing the lesion in the very early phase, before scar tissue starts forming, and we follow up with stem cells.”
In the case of suspensory ligament injuries, Fortier reaches straight for a combination of stem cells and extracorporeal shock wave therapy, adding that she’s had limited success with PRP- or IRAP-based products for treating these lesions.
Another classic condition for which regenerative medicine comes to the rescue is osteoarthritis, a painful degenerative joint disease that has no cure. Owners can choose between PRP, ACS, and SCT to help manage their horses’ joint pain. Studies support the use of each of these products; however, individual equine veterinarians have their preferences.
“I use leuko-reduced PRP for joints because this approach is supported by the highest level of evidence in people for mild-to-moderate arthritis,” Fortier says.
Watts prefers SCT to PRP or ACS. “At Texas A&M University, we are back to using stem cells in joints,” she explains. “With optimized preparation methods we are seeing predictable and sometimes almost miraculous results in joints with osteoarthritis and joints with damage to the articular cartilage.
“What we need is more research to develop the ideal treatment regimens for stem cells, including which cases are the best candidates,” she continues. “Currently we are injecting high-motion joints that have failed to respond to corticosteroid injections, or have severe cartilage injury, with autologous (self) stem cells every three weeks for a minimum of three treatments. Whether we need to follow up with repeat stem cell injections after this protocol is not known. We need more research, and we need an FDA-approved stem cell product.”
“What is important to remember is that we have choices: PRP, IRAP, and stem cells,” says Fortier. “There are no head-to-head comparisons for these therapies in tendon, ligaments, or joints in horses, so opinions will vary between veterinarians depending on their personal experiences.”
Further, the exact treatment regimen and associated costs will depend on the severity of the disease and how soon the horse receives treatment.
“If a horse is treated in the first couple of weeks of developing a tendinopathy, then only one treatment might be needed,” says Fortier. “Regenerative therapies and rehabilitation need to be applied in the early phase, ideally in the zero- to three-week window after injury, before scar tissue starts to form.”
Other Conditions
Because of regenerative techniques’ proven and perceived effects in horses with musculoskeletal injuries, veterinarians and researchers are exploring their use in other settings, as well. These uses, however, remain quite experimental but might have a great deal to offer, especially for conditions that have, to date, remained resistant to standard medical approaches. Consider some of the following:
- SCT or ACS for modulating persistent mating-induced endometritis (inflammation of the uterine lining).
- SCT for systemic inflammatory conditions such as endotoxemia, equine asthma, inflammatory bowel disease, and uveitis (a type of eye inflammation).
- SCT for equine metabolic syndrome, which is characterized by obesity, insulin dysregulation, and laminitis.
The rationale behind using stem cells in these settings is to promote damage repair, renew/reverse aging of certain cells, improve tissue and organ structure and function, and promote the use and excretion of metabolites. With immune-mediate diseases, for instance, stem cells could potentially reduce immune cell activation (e.g., with uveitis) and in others modulate inflammation.
What’s Next?
The field of regenerative medicine, although still in its infancy, has exploded since its introduction in the late 1960s. Despite the widespread use of PRP, ACS, and SCT, barriers exist pertaining to their use, including clear-cut instructions on how to prepare and administer them properly.
“I think with optimized preparation methods we will hopefully have an approved SCT for horses in the U.S. soon,” says Watts.
Looking further into the future, Fortier suggests the next type of regenerative product for horses will be a “secretome.”
“Essentially, a secretome would include all the bioactive factors that stem cells secrete to elicit the desired clinical effect,” she says. “This way, we will have a cell-free product that delivers all the benefits that SCT has to offer but will be a consistent product. By FDA regulations, secretome will be a drug and will need to clear all the associated regulatory pathways to become available for use.”
Fortier cautions that “there are no secretome products on the market right now, but plenty of companies are suggesting that their product contains secretome. Owners and veterinarians should be very wary of these products and, in fact, should ask the company for their IND (investigational new drug) number. This number will indicate that the company has some evidence that their product contains secretome and that they have filed with the FDA to be able to investigate the efficacy of their secretome drug in your horse.”

Written by:
Stacey Oke, DVM, MSc
Related Articles
Stay on top of the most recent Horse Health news with












