Vets Discuss How They Use SAA in Equine Practice
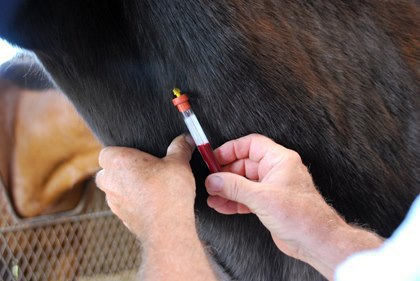
Does your practice routinely use serum amyloid A (SAA) testing and, if so, how? Are you looking to implement this test into your toolbox but aren’t sure how to go about it? Two internal medicine veterinarians answered these questions during a Table Topic discussion at the 2018 American Association of Equine Practitioners convention, held Dec. 1-5, in San Francisco, California.
Nicola Pusterla, DVM, PhD, Dipl. ACVIM, professor of medicine and epidemiology at the University of California, Davis, School of Veterinary Medicine, and Laura H. Javsicas, VMD, Dipl. ACVIM, of Rhinebeck Equine LLP, in New York, co-mediated the session. They kicked it off with a brief review of SAA basics.
What is SAA?
Pusterla quickly reminded attendees that SAA—referred to as an acute-phase protein produced by the liver—essentially acts as a marker of inflammation. He highlighted the fact that while SAA is a powerful indicator that inflammation is present, the test can’t tell you what’s causing the inflammation or, importantly, where it is
Create a free account with TheHorse.com to view this content.
TheHorse.com is home to thousands of free articles about horse health care. In order to access some of our exclusive free content, you must be signed into TheHorse.com.
Start your free account today!
Already have an account?
and continue reading.

Written by:
Stacey Oke, DVM, MSc
Related Articles
Stay on top of the most recent Horse Health news with












