Figuring Out Limb Fractures in Horses
- Topics: Article, Fractures, Horse Care, Injuries & Lameness, Lameness, Sports Medicine
Type of fracture, diagnosis, and treatment dictate a horse’s chances of recovery

Finding a horse unable to bear weight on a limb can be a nightmare. And when your veterinarian says the word fracture, you might immediately anticipate the worst-case scenario: euthanasia. But don’t jump to conclusions.
With all the advancements in modern veterinary medicine, fractures are no longer death sentences for horses. Veterinarians can repair and rehab many limb fractures, and the horse might even be able to return to work.
Dean Richardson, DVM, Dipl. ACVS, head of surgery at the George D. Widener Hospital for Large Animals at the University of Pennsylvania’s New Bolton Center, in Kennett Square, says the biggest horse owner misconception is that you can’t treat a fracture.
“You need to get every case evaluated separately,” says Richardson. “Just because somebody has experience with a fracture that couldn’t be repaired doesn’t mean that the one you’re looking at can’t be repaired. Some of them have a terrible prognosis, and some have an excellent prognosis. Also, not every fracture in the horse needs surgery.”
Let’s look at types of limb fractures and how to handle them.
Fracture Diagnosis
The first thing to understand about fractures is that they encompass a wide range of bone injuries, from small chips to large fragments called slab fractures. Common types include:
- Simple Only one crack in the bone.
- Comminuted Splintered or having many pieces of separated bone.
- Incomplete A fracture on only one side of the bone.
- Complete A full break that results in separated bone fragments.
- Displaced When bone fragments have moved out of their original position.
- Stress Small, incomplete fractures.
- Star Multiple cracks radiating from a central area.
- Articular A fracture involving a joint.
- Closed Without a wound.
- Open With a wound.
A fracture can produce localized heat, pain, and swelling—either alone or in combination with lameness. These are typically the first clinical signs you’ll notice, especially if you did not see the injury occur.
The presence of a wound can throw some owners off as to the underlying cause of a horse’s pain or lameness, says Laurie Goodrich, DVM, PhD, Dipl. ACVS, professor of surgery and lameness at Colorado State University’s Equine Hospital and Orthopaedic Research Center, in Fort Collins.
“Sometimes they assume that the wound is the primary scenario that is causing the soreness, but it’s important for them to be aware that the bone underneath it can be affected,” she says.
While lameness is the most relevant clinical finding, not every lame horse has a fracture. “You can imagine how many horses have come in over the years to any hospital with an owner convinced the horse has broken his leg, when in fact what it has is a hoof abscess,” says Richardson. “The thing we always teach veterinary students is that if you have a severely lame horse, there are two differentials (conditions to consider that cause similar clinical signs): a fracture or an infection.”
An accurate diagnosis is important so the veterinarian can stabilize the limb properly to prevent further damage. Diagnostics have come a long way due to most vets having digital radiograph (X ray) units, allowing them to detect fractures in the field, says Goodrich.
Because it can be more difficult to get a good radiograph as you move up the limb, due to the additional muscle tissue, Goodrich says some veterinarians might opt to perform an ultrasound.
Dr. Dean Richardson
Immediate Care of the Horse
Both Goodrich and Richardson emphasize that no one should move an injured horse unless absolutely necessary. If a horse needs to be moved out of a dangerous situation or the hot sun, for instance, move him as short a distance as possible.
“A horse can do a lot of damage, and it can be very anxiety-provoking to the horse if you try to move him when you’ve got an unstable limb,” says Richardson.
The veterinarian will give the horse a non-steroidal anti-inflammatory drug, such as phenylbutazone (Bute), flunixin meglumine (Banamine), or firocoxib (Equioxx), to control pain and inflammation, says Richardson.
“They are always given to a horse with a fracture, because they are not going to provide such intense pain relief that the horse is going to worsen the fracture by walking on it,” he adds.
Goodrich suggests starting antibiotics right away if dealing with an open fracture, because a wound makes way for infection.
The veterinarian might also sedate the horse to calm him, especially if applying a splint, although Richardson warns against using strong pain medications or heavy sedation that could make the horse too difficult to move onto a trailer after splinting.
He advises horse owners to let the veterinarian splint the horse. “The average horse owner doesn’t often do an appropriate job because you have to understand the anatomy of what you are splinting,” he says.
The veterinarian chooses a splinting method based on the affected area and personal preference to immobilize the fracture and provide support so the horse can walk and stand during transport to a referral hospital.
“Sometimes you don’t even immobilize the fracture,” Richardson says. “You’re just immobilizing a part of the limb (so that it) allows the horse to walk on it. If you have a fractured ulna (which, with the radius, forms the horse’s forearm), all you have to do is put a splint that stabilizes the carpus (knee), and that makes an enormous difference to the horse. When you splint a horse with an ulnar fracture properly and just splint his knee, you can see them almost visibly sigh with relief because all of a sudden they can bear weight on their limb.”
After a veterinarian has examined and, if needed, splinted the horse, you can trailer him to a clinic for treatment. Transporting the horse is the most dangerous part of dealing with a limb fracture, especially if you haven’t supported and stabilized it properly.
The smoothest ride for a horse with a fracture is a gooseneck trailer with a ramp. Richardson says he has seen plenty of well-meaning horse owners take trailer partitions out to give the horse as much room as possible to lie down, but that’s the wrong thing to do. Instead, he advocates keeping the partitions and using the tightest possible space; this allows the horse to use his body to help support himself by leaning against something from left to right and front to back. Don’t restrict his head and neck, however.
With forelimb fractures, ship the horse facing backward, if possible, so if you must brake suddenly, all his weight will shift to the hindquarters. Ship the horse with hind-limb fractures facing forward.
Shipping a foal that’s sustained a fracture is a different situation. Richardson recommends sedating foals heavily and shipping them in recumbency (lying down) with their dams standing.
At the Hospital
Once the horse has arrived at the hospital safely, the veterinary staff will evaluate him and make a plan to repair the limb. The veterinarian might perform additional diagnostics, such as another round of radiographs.
“Just because the fracture looked a certain way when it was sent (to the hospital) doesn’t mean that it’s necessarily going to be unchanged after transportation,” says Richardson. “Any type of complicated fracture that we can get a CT scan on, we will do that because that gives you a far superior ability to plan the surgical procedure if you have three-dimensional images.”
He adds that he doesn’t find MRI as useful for assessing a fracture.
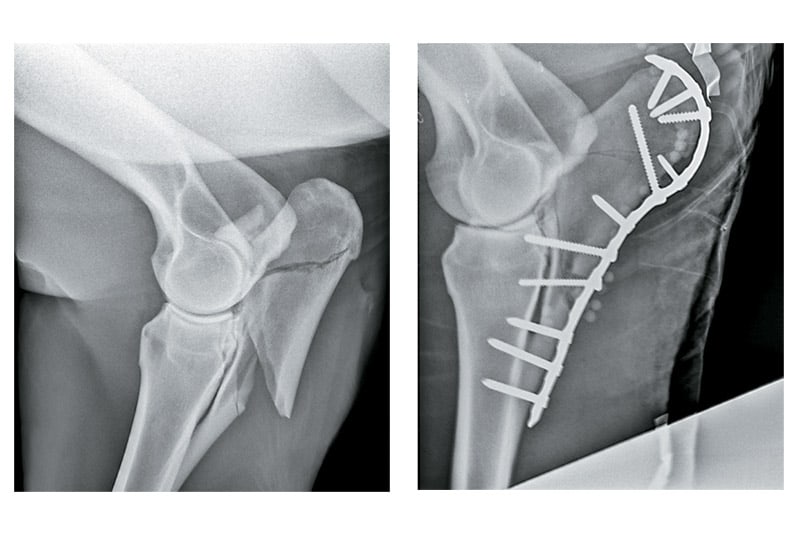
Surgery often involves internal fixation with stainless steel screws and plates. Goodrich says veterinarians recommend this type of surgery for horses that are very uncomfortable and/or have a fracture that is displaced or at risk of displacing.
She believes locking plates (in which screws lock into the plates used to stabilize a fracture) have completely revolutionized fracture repair in horses by allowing surgeons to stabilize and maintain bones they couldn’t previously. They can also maintain stability in the face of infection (e.g., with open fractures), says Goodrich, which has improved prognoses. This is due to the mechanics locking plates can maintain throughout wound infection treatment.
Advancements in treating infected fractures, which she says comprise 20-30% of cases, have been huge. One involves using a tourniquet that allows for intravenous (IV) antibiotic administration. In addition, she says, “antibiotics can be added to bone cement and applied next to a fracture,” allowing the drugs to reach effective levels at the fracture and implant sites.
When it comes to healing, however, Richardson says there’s nothing better than bone. “Bone is the only thing in your body that truly heals, and bone almost always ends up getting stronger over time, not weaker,” he says. “So rehabilitation in horses with fractures is almost always based on managing the other tissues—the muscle, tendons, joints, ligaments—and then just keeping mobility in those structures, because the bone is going to heal.”
Healing and Prognosis
Bone healing in adult horses typically takes at least four months, whereas foals heal faster. Veterinarians might recommend rehabilitation exercises (e.g., mobilization, swimming, water treadmills) to restore mobility to joints and rebuild muscle function.
Some equine limb fractures have better outcomes than others. Prognosis can depend on many factors, says Richardson, including the horse’s expected use, age, size, whether the fracture restricts mobility, if the fracture is displaced, etc. One of the biggest factors affecting prognosis, however, is the fracture’s location.
Fractures that typically have good prognoses include:
- Those of the ulna’s olecranon process, which is the point of the elbow. Richardson estimates that 90% of horses survive this common fracture, with many returning to full athletic function.
- Chip fractures, which surgeons can remove arthroscopically. “You can have a very high expectation that the horse goes back to full athletic soundness for many, many types of those,” Richardson says.
- Fractures repaired surgically using lag screw fixation to compress fragments together. In most cases the hardware remains in the horse for his lifetime. These horses can return to full function.
- Simple fractures with simple repairs.
Fractures with poorer prognoses include:
- Displaced radius (the forearm bone extending down from the elbow) fractures, which Richardson says are expensive and very difficult to repair.
- Moderate or severe articular fractures requiring surgery to fuse the affected joint to reconstruct it. The horse can live a good life but might never return to full athletic function, says Richardson.
- Open fractures. “When you place implants to stabilize a fracture that’s contaminated, then the likelihood of having an infection is almost guaranteed,” says Goodrich.
- Complex fractures with complicated repairs.
One of Richardson’s most important reminders to owners is to get radiographs for any horse kicked above the knee that’s not sound. With a correct diagnosis and stall rest, horses with incomplete fractures of the radius can recover and go back to full work with no problems.
“But if you take that same horse and think, ‘Oh, that’s nothing,’ and turn it out, that’s a horse that can come in with its radius completely separated and displaced or catastrophically fractured, and then you’ve got a $15,000 to $20,000 (procedure) with a poor expectation of a good outcome,” he says.
Take-Home Message
Fracture repair in horses has come a long way. Having a veterinarian splint the injury properly in the field before transporting him to an emergency clinic is critical to success, our sources say. With advancements in treatment, many horses with fractures either return to partial or complete athletic function or can be used as breeding stock. This can provide horse owners with hope they can save their horses and give them functional, happy, and comfortable lives.
[/et_pb_text]
Written by:
Sarah Evers Conrad
Related Articles
Stay on top of the most recent Horse Health news with
















