Getting a Handle on Scratches in Horses
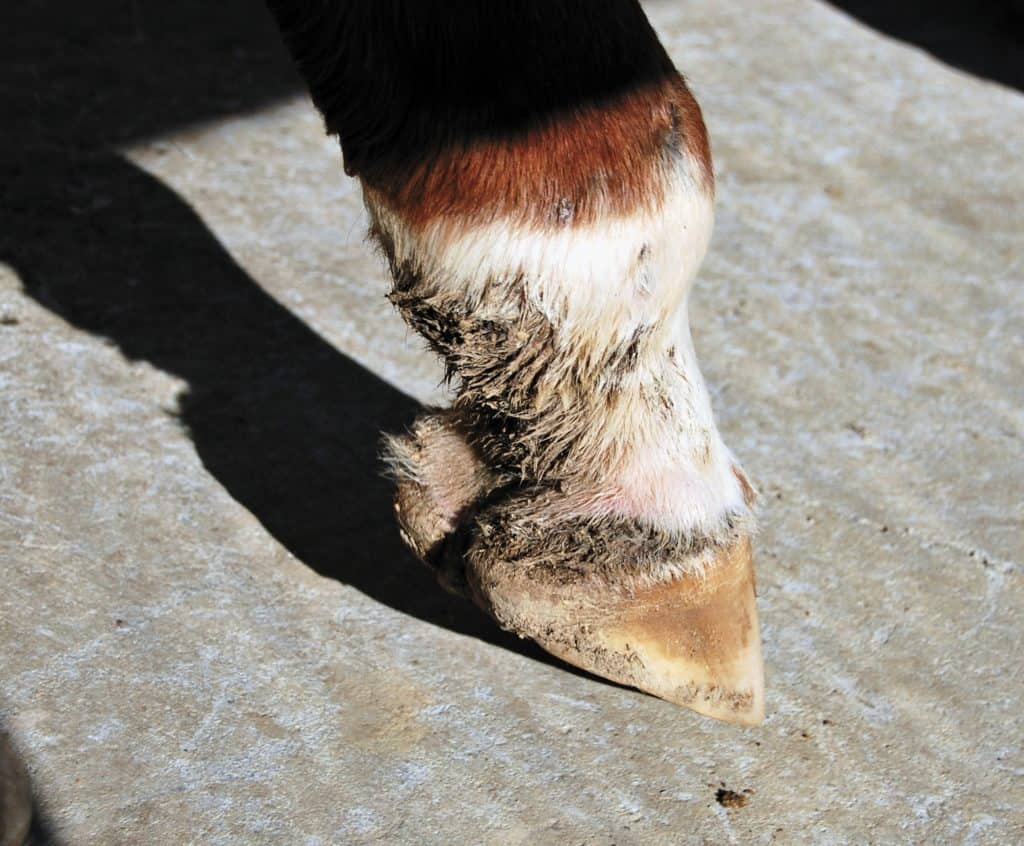
Scratches, or equine pastern dermatitis (EPD), is not a disease but, rather, a cutaneous reaction pattern. Veterinarians and owners must address the primary, predisposing, and perpetuating causative factors for a successful outcome. Note that treating the predisposing and perpetuating factors is just as important as addressing the primary cause.
Clinical Signs and Pathogenesis
Scratches can affect any breed, but is most prevalent in draft horses due to long pastern hair (“feathers”). It most commonly affects the rear aspect of the hind pasterns and especially nonpigmented skin. Without treatment the lesions can spread to the front of the pastern and fetlock. Clinical signs vary, but initially owners might notice edema (fluid swelling), redness, and scaling, rapidly progressing to oozing, hair matting, and crusting. If the cause is vasculitis (blood vessel wall inflammation), ulcers might form on the skin. Secondary bacterial infection is a common complication and can perpetuate the signs. In chronic cases skin can thicken and fissure due to constant movement and flexion in this area. The lesions are often painful.
Diagnosis
In a veterinarian’s detailed history, he or she should include the horse’s age, month of onset, whether the scratches is seasonal and/or pruritic (itchy), if there has been overzealous use of topical medications or home remedies, and response to prior treatment. He or she should also inspect the environment because wet or chemically treated bedding, along with muddy pastures and insects, can cause allergic contact dermatitis (from allergens touching the skin). If in-contact animals or humans are also affected it might indicate an infectious or zoonotic condition such as dermatophytosis (fungal infection). Another diagnostic rule-out is parasites—chorioptic mange is a common cause of pastern dermatitis in draft horses. But more commonly the cause of pastern folliculitis (a pus-forming skin infection) is bacterial, with Staphylococcus aureus and Dermatophilus congolensis as the culprits. Horses with white extremities can suffer from photosensitization or immune-mediated pastern leukocytoclastic vasculitis (PLV), both exacerbated by UV light. Based on the information provided, your veterinarian might pursue specific diagnostics such as skin scrapings, fungal cultures, tape impression, skin cytology, skin biopsies, allergy testing, or bloodwork.
Treatments

After your veterinarian identifies the causative factors, it’s time to pursue appropriate therapy. Here are some environmental changes you can make:
- Avoid turning affected horses out in pastures with mud, water, or sand, which can worsen the condition.
- Keep horses in clean, dry stalls during wet weather.
- Do not turn horses out until the morning dew has dried.
- If you suspect contact allergic dermatitis, try an alternate source of bedding that isn’t treated or aromatic.
- Clip heavy feathers over the pasterns to reduce moisture retention.
- If you suspect PLV, avoid UV light exposure by stabling the horse between 10 a.m. and 4 p.m. and/or wrapping the affected legs.
- Clean affected skin immediately after exercise using an antiseptic shampoo.
Clinical treatments include topical and systemic therapeutics. Secondary infections with Staphylococcus spp are common and can complicate diagnosis. Available antibacterial shampoos typically contain ethyl lactate, accelerated hydrogen peroxide, 2% benzoyl peroxide, or 2% chlorhexidine. If lesions are exudative, apply astringent solutions, such as lime sulfur or aluminum acetate.
Ointments such as silver sulfadiazine, fucidin, and 2% mupirocin ointment are available for treating localized bacterial infections. To treat bacteria, dermatophytes, or mites owners can apply lime sulfur dips and spray. Enilconazole spray or dip, along with miconazole shampoo with or without chlorhexidine shampoo, can be used to treat fungal infections.
Sprays such as hydrocortisone aceponate or 0.015% triamcinolone can be used in conjunction with systemic immunomodulators to treat allergic and immune-mediated conditions such as PLV. In addition, veterinarians have noted success applying 0.1% topical mometasone, 1% betamethasone, or 0.05% aclometasone creams or ointments to lesions. Horses with immune-mediated conditions might also require immunosuppressive doses of dexamethasone or prednisolone.
Antiparasitic approaches for Chorioptes include ivermectin, topical eprinomectin solution, selenium sulfide shampoo followed by lime sulfur, and fipronil spray.
Written by:
Anthony Yu, DVM, MS, Dipl. ACVD
Related Articles
Stay on top of the most recent Horse Health news with















