Insect-Borne Equine Diseases: Q&A
Find answers to questions about equine infectious anemia, Potomac horse fever, parasites, and more.
Share
ADVERTISEMENT
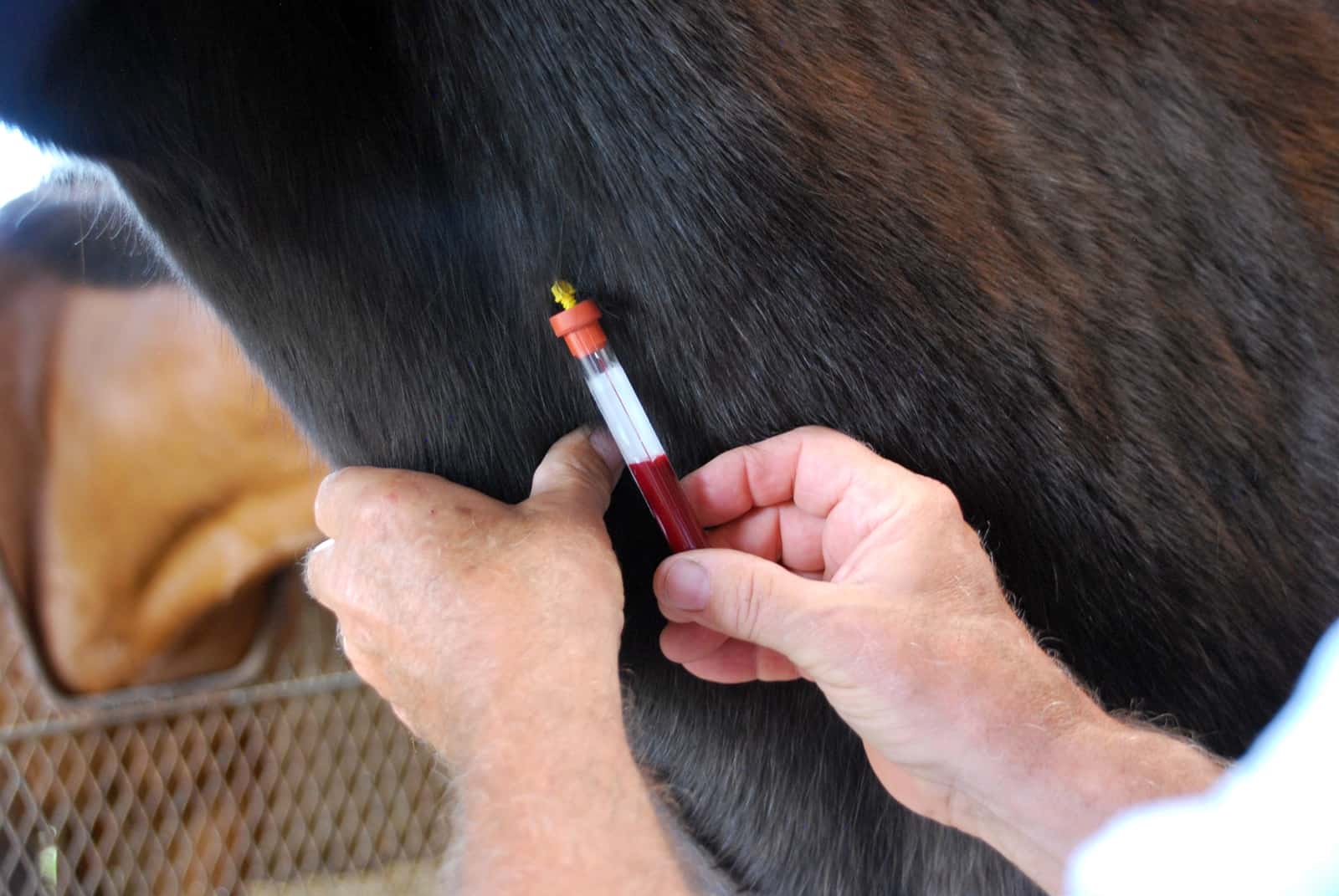
A Coggins test screens the horse’s blood for antibodies against EIA’s causative virus. | Photo: Alexandra Beckstett/The Horse
During the 2019 University of Kentucky (UK) Equine Showcase, held Jan. 26 in Lexington, Rebecca Ruby, BVSc, Dipl. ACVP, of the UK Veterinary Diagnostic Laboratory, educated horse owners about important equine diseases carried or caused by insects.
What is equine infectious anemia (EIA) and how does a horse get it?
EIA is caused by a virus that integrates into the horse’s DNA and results in life-long infection. There is no vaccine and no cure for the disease
Create a free account with TheHorse.com to view this content.
TheHorse.com is home to thousands of free articles about horse health care. In order to access some of our exclusive free content, you must be signed into TheHorse.com.
Start your free account today!
Already have an account?
and continue reading.
Share
Related Articles
Stay on top of the most recent Horse Health news with










