Is Ultrasound Useful for Diagnosing Hind-Limb PSD?
Sue Dyson, MA, Vet MB, PhD, DEO, FRCVS, head of clinical orthopaedics at the Animal Health Trust Centre for Equine Studies, in Newmarket, England, recently evaluated whether ultrasonography is a reliable method for diagnosing PSD. She shared the results at the 2015 American Association of Equine Practitioners’ Convention, held Dec. 5-9 in Las Vegas.
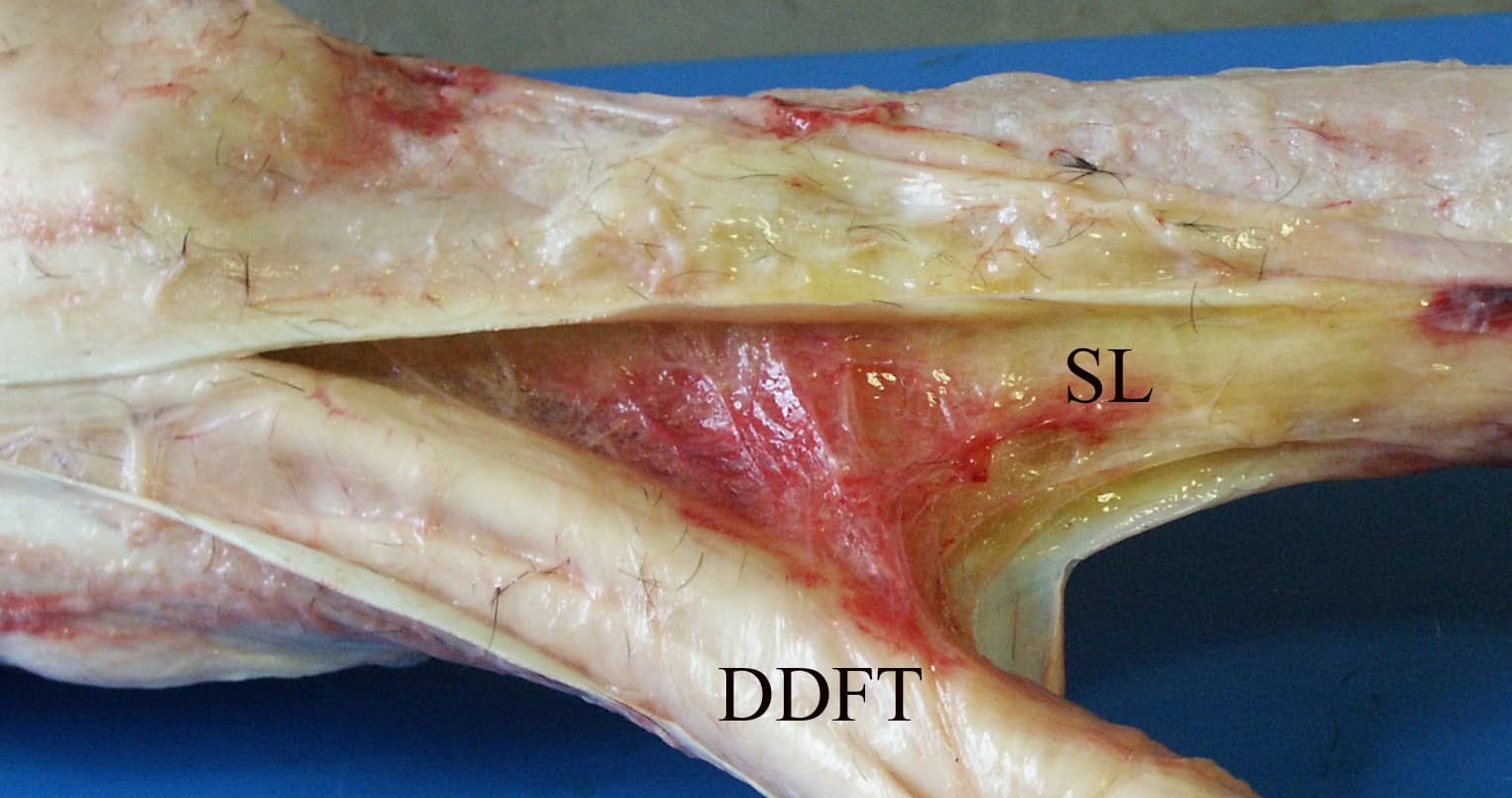
Horses with PSD have inflammation and tissue damage in the upper part of the suspensory ligament, a structure that connects to the top back of the cannon bone, divides into two branches which attach to the proximal sesamoid bones, and lies under the superficial and deep digital flexor tendons and the check ligament. Traditional treatment approaches generally involve an extended, expensive period of confinement or inactivity. Further, researchers have determined that the prognosis for hind-limb PSD following conservative therapy (which generally consists of rest, with or without shockwave therapy and treatment with drugs such as corticosteroids) alone is poor, with only 14% of horses resuming full work without lameness for more than a year. Surgeons also treat PSD with procedures such as neurectomy of the deep branch of the lateral plantar nerve (cutting or transecting the nerve) and fasciotomy (ligament splitting) or desmoplasty (a procedure in which numerous small longitudinal stab incisions are made in the ligament).
Dyson said an earlier study’s results had suggested that diagnostic ultrasound is unreliable for detecting hind-limb PSD and that MRI is vastly superior and should be the gold standard for diagnosis. However, MRI is considerably more expensive than ultrasound, and not every veterinarian has ready access to it. So she and colleagues set out to compare ultrasound findings with post-mortem gross dissection and histology findings (cell structure under a microscope).
In the first part of their two-part study, the team evaluated 19 horses diagnosed with hind-limb PSD, euthanized for reasons unrelated to the study. Based on ultrasound examination prior to euthanasia, the team graded the severity of each horse’s PSD as mild, moderate, or severe. After the horses were euthanized, the team examined 37 limbs grossly and 36 suspensory ligaments histologically (one of the 37 ligaments was excluded due to processing problems). They graded the suspensories on a four-point scale (0 being normal and 3 indicating severe abnormalities). They also examined the suspensory ligaments of 10 control horses with no evidence of PSD post-mortem.
Key findings from the first part of the study included:
- Lameness was detectable in 47% of the horses when they were presented in hand and in 68% of horses when longed; all the horses were lame when presented under saddle or in harness;
- Most of the horses’ lamenesses were characterized by a lack of hind-end impulsion;
- Pre-mortem ultrasound examination revealed evidence of moderate PSD in 31 limbs and severe PSD in seven limbs;
- Ultrasound also predicted the presence of adhesions (restrictive bands of scar tissue that can complicate healing) in four limbs;
- On gross necropsy, the veterinarians did not identify adhesions in any of the nonlame (control) limbs;
- Gross examination revealed adhesions between the suspensory ligament and adjacent soft tissue structures in 27% of the lame limbs, despite the fact that with ultrasound they only predicted adhesions in four limbs;
- Further, the team found that tough adhesions had formed between the suspensory ligament and cannon bone in 10 limbs, which ultrasound exams had not predicted;
- Histology performed on control limbs without PSD revealed no abnormalities; and
- However, Dyson and her team noted numerous abnormalities in PSD limbs: Collagenous tissue was abnormal in 69%, muscle tissue was abnormal in 97%, adipose (fat) tissue was abnormal in 44%, neural abnormalities were observed in 64%, and vascular changes (changes in blood supply to the area) were evident in 8%.
Dyson said that one lame limb had no histologic abnormalities at any of the sampled sites; however, the horse had tough adhesions between the suspensory and the deep digital flexor tendon in several locations.
In the second part, the team evaluated seven other horses with PSD; three of those presented with recurrent lameness following previous surgical treatment of PSD, and four had suspected adhesions between the upper suspensory ligament and the cannon bone, based on ultrasound findings. Those horses were euthanized for reasons unrelated to the study, and the team carried out gross necropsies without histology. In this part of the study, the team determined that while ultrasound accurately predicted some adhesions, others went undetected and were only confirmed on necropsy.
Ultimately, Dyson determined that good-quality ultrasonography is reasonably reliable for detecting PSD when judged against post-mortem findings as the ultimate gold standard, but it underestimates the presence of adhesions. Researchers have not previously described adhesions between the suspensory ligament and adjacent soft tissues or bones in the literature and could be a reason why some horses do not respond to treatment, she added, because that area has not been treated.

Written by:
Erica Larson
Related Articles
Stay on top of the most recent Horse Health news with















