What You Need to Know About Equine Osteoarthritis
- Topics: Arthritis & Degenerative Joint Disease, Arthritis & Degenerative Joint Disease, Basic Care, Bone & Joint Problems, Horse Care, Injuries & Lameness, Joint Supplements, Lameness, Medications, Older Horse Care Concerns, Pain Management, Sports Medicine, Sports Nutrition, Working With a Veterinarian

Learn more about this crippling condition that affects horses of all breeds, disciplines, and ages
You, the horse owner, asked, and we listened: Arthritis is an extremely common condition that continues to frustrate you, in terms of both short- and long-term management. Before answering some of your top questions about the latest developments in this field, let’s review the condition.
Arthritis simply means joint inflammation. In horses several types of arthritis can occur, with causes ranging from infection to age and years of athletic use. Typically, however, owners use the word arthritis in lieu of osteoarthritis—a chronic, progressive, painful degeneration of the cartilage lining the ends of long bones inside joints, as well as the underlying bone and soft tissues.
Osteoarthritis (OA), which used to be known as degenerative joint disease, can affect any joint where two cartilage-covered bones meet—called an articular joint. In sport/athletic horses we often think of OA affecting the joints in the limbs, such as hocks, knees, stifles, and fetlocks. Classic signs include heat, swelling due to excess joint fluid, lameness/pain, stiffness, deformation caused by bony changes, and crepitus—that popping, grinding, and crackling sound and sensation in an affected joint.
“The knees, (fetlocks), hocks, and stifles are in fact some of the most common joints diagnosed with OA in horses, but any articular joint can be impacted, including the multitude of individual joints along the length of the spine, hips, and even the jaw or temporomandibular joint,” says Sheila Laverty, DVM, MVB, Dipl. ACVS, ECVS, equine surgery professor and equine surgery service chief at the University of Montreal’s School of Veterinary Medicine, in Saint-Hyacinthe, Quebec. Laverty also heads the school’s Comparative Orthopaedic Research Laboratory, which she says is committed to improving joint health in all species.
Armed with the basics, here are the common questions regarding OA in horses you said you needed answered at TheHorse.com.
Q: How can I gauge my arthritic horse’s pain levels?
This is a fantastic question because OA ’s prevailing clinical sign is pain manifesting as lameness. The most common method of assessing lameness is a veterinary lameness exam, generally using the American Association of Equine Practitioners’ lameness scale, as well as flexion testing and anesthetic blocks (regional or in the joint, if possible) to accurately determine the site of pain. Radiographs (X rays) reveal typical OA lesions, but none might be evident in the early stages because cartilage is not visible on radiographs. Horses with mild OA often appear stiff when emerging from the stall or starting work before warming up and looking more comfortable. More severe signs include swelling, heat, and persistent lameness, which can preclude comfort and athleticism.
To complicate the situation, OA is one of those conditions that people tend to assume a horse has simply because it’s so common. However, deciding a horse has any medical condition and treating it without consulting a veterinarian can have serious consequences, delay appropriate treatment, and drain valuable owner resources.
“Assuming a horse is suffering from OA can be dangerous, as there are actually several other conditions that present similarly to lameness associated with OA,” warns Laverty. “The list is long and can (include) a variety of conditions affecting the bones and soft tissues.”
Q: How can I keep my arthritic horse comfortable?
Currently, options for managing pain in horses with OA remain limited, even though a plethora of pharmaceutical and nonpharmaceutical options exist. Common pharmaceutical approaches include:
- Non-steroidal anti-inflammatory drugs such as phenylbutazone (Bute) administered by mouth, usually daily; or
- Injectable products that contain hyaluronic acid or polysulfated-based active ingredients such as polysulfated glycosaminoglycan (PSGAG) and pentosan polysulfate sodium (PPS).
Recently, Laverty and colleagues dove deeper into how OA causes pain and lameness.
“While it may be difficult to impossible to differentiate clinically, pain can actually be classified as one of three broad ‘types,’ and each appears to contribute to the pain associated with OA,” she says.
Those three types include:
- Nociceptive pain, which is caused by activation of pain receptors in the joint secondary to abnormal movements associated with OA.
- Inflammatory pain, resulting from the release of inflammatory mediators that impact a variety of surrounding joint tissues. Inflammatory mediators can also “prime” the nociceptive pain receptors in joint tissues, making them more sensitive than normal and increasing pain levels.
- Neuropathic pain, caused by damage to specific regions of the horse’s nervous system that perceive pain.
“In the past, we assumed that the pain associated with OA was primarily nociceptive in nature, but we now appreciate that to adequately control the discomfort associated with OA, all three types of pain may need to be addressed,” Laverty says.
“It is fascinating that the exact tissue source of the pain sensation is unknown in the case of OA,” she adds. “Articular cartilage does not have nerves, whereas the soft tissues such as ligaments and synovial membranes and bone are innervated.”
While researchers continue to search for better pharmaceutical treatment options for OA, owners often elect to pursue nonpharmaceutical approaches. Joint supplements and other options (which we’ll discuss in more detail) remain popular, though researchers on several recent studies emphasize the importance of addressing weight management.
The number of overweight and obese horses mirrors the obesity epidemic in humans and other companion animals. In a recent study Canadian researchers reported that approximately one in three domestic horses is considered not just overweight, but obese.
Dr. Erin Contino
Erin Contino, MS, DVM, Dipl. ACVSMR, of Colorado State University’s Orthopaedic Research Center, in Fort Collins, says data generated in human and dog studies firmly support that extra weight negatively affects arthritis patients.
“Every pound of extra weight in humans results in a 4-pound increase in forces on the knee,” she says. “And after an 11-18% decrease in body weight, dogs with hip OA experienced less lameness and increased life spans. Because OA is comparable among dogs, humans, and horses, similar benefits associated with weight loss and OA would be expected in horses.”
Achieving weight loss in horses, similar to other mammals, boils down to expending more energy than what is being consumed. In most cases a combination of exercise and decreased feed intake forms the foundation of weight management. One of the key factors for success is owner recognition of appropriate body weight, which can be challenging.
A management change that can encourage weight loss, as well as help your arthritic horse feel better, is increased pasture turnout. Movement minimizes the classic stiffness horses with joint disease might display at the start of exercise. Also avoid intermittent exercise sessions. If possible, continue working horses with OA routinely—even just lightly—to keep them fit and pliable.
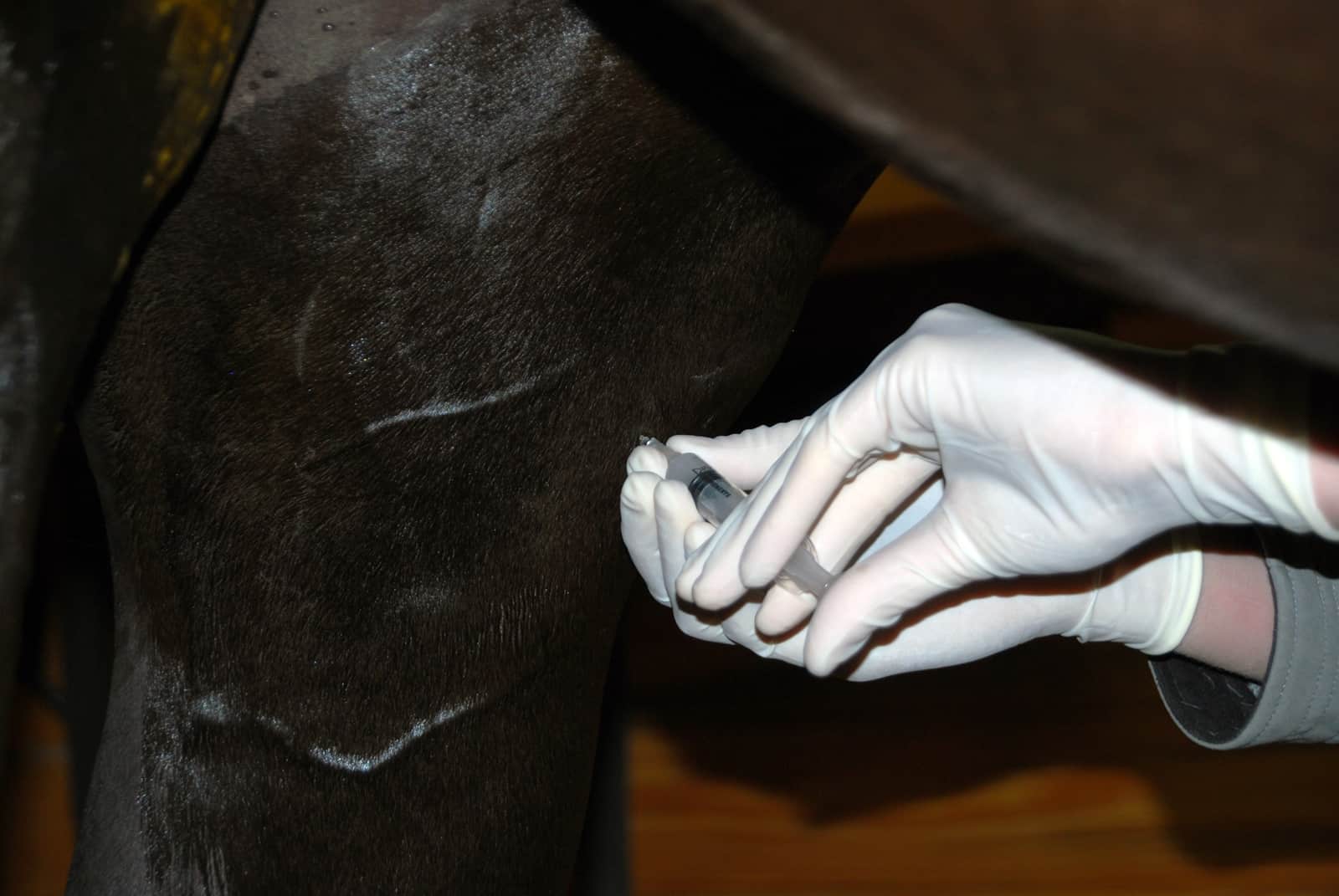
Q: What should I know about joint injections?
Falling under the umbrella of pharmaceutical management of OA, joint injections remain a popular option, particularly for owners of equine athletes that are still competing.
“Intra-articular (in the joint) therapy often provides the most ‘bang for your buck,’ but only when used once an accurate diagnosis of OA has been made while also assessing the affected joint, severity of disease, age and use of the horse, and potential underlying causes or contributing factors,” says Contino.
Products typically used intra-articularly include corticosteroids, which, says Contino, remain the “cornerstone for managing joint disease and for a good reason.” These products include betamethasone, methylprednisolone acetate, and perhaps the king of the hill, triamcinolone. Product selection varies depending on your veterinarian’s preference, the amount to be administered, and if it’s a high- or low-motion joint.
Other injectable products include sodium hyaluronate (hyaluronic acid), polysulfated glycosaminoglycan, bisphosphonates (only FDA-approved for managing horses diagnosed with disease involving the navicular apparatus), and biological or regenerative therapies such as stem cells, IRAP (interleukin-1 receptor antagonist), and platelet-rich plasma. The use of stem cells and platelet-rich plasma for OA remains relatively unproven at this point, as no real treatment protocols or rules on how to use these products exist. It is, however, a very active field of research, and some veterinarians currently use these technologies to treat horses with OA.
The decision when to pursue intra-articular treatments must be made on a case-by-case basis with your veterinarian. “The use of intra-articular medication is not without risk,” says Laverty. “An infection may arise following injection and can be catastrophic for the joint and horse.”

Q: With all the oral joint supplements on the market, how do you know which ones work?
Several studies summarize important tips for selecting quality joint supplements that are most likely to contain the type or amount of ingredient listed on the product label.
“Of the wide array of joint supplements available to horse owners, independent laboratory analyses reveal that the majority of these products fall short of the labeled amounts,” says Contino. “This creates a buyer-beware market, and many veterinarians are left making recommendations based on limited research from the company and/or based on a company’s reputation.”
Research-proven ingredients include glucosamine, chondroitin, avocado-soybean unsaponifiables (ASU), green tea extracts, fish oils containing the omega fatty acids EPA and DHA, among others. Products that do not contain adequate or appropriate levels of quality ingredients can delay treatment and negatively impact arthritic horses’ quality of life.
The message veterinarians continue to relay is this: Do your research before buying a supplement, consult your veterinarian or equine nutritionist, follow the product’s label directions, and critically evaluate your horse’s condition.
“Keep your eyes open for newer ingredients and information on joint supplements for OA,” says Contino. “Recently, curcumin, turmeric, and other polyphenolic plant extracts such as resveratrol and grape seed extracts have been studied, (with) some of those, particularly resveratrol, showing promise for supplemented horses.”
Q: Are there noninvasive or more conservative ways to manage my horse’s arthritis?
Lack of adequate pain control, costs associated with treatment, and undesirable side effects associated with commercial pain medications (e.g., gastric ulcers, diarrhea, weight loss, concerns about joints flares/infections) make horse owners covet alternative pain management strategies. These options include the nutritional supplements described, as well as acupuncture, shock wave therapy, and physical/rehabilitation therapy.
“What we have learned from decades of work in human medicine is that many types of arthritis can benefit from correct movement to help realign the joint,” says Sheila Schils, PhD in kinesiology/biomechanics. She is co-founder of and clinician at EquiNew, in River Falls, Wisconsin, which specializes in therapeutic modalities. “This realignment is necessary due to the fact that incorrect biomechanics of the joints can cause unequal pressure and eventual breakdown of the joint, causing pain.
“A good analogy is what happens if the wheels of your truck are not sitting on the axle straight and balanced; the tires will wear unevenly,” she adds. “The outer edge of the tire can look like new, while the inner edge of the tire is worn down to the steel belts. Therefore, just changing the tires will not solve the problem. Instead, you need to fix the alignment of the wheel on the axle. This is the foundation behind the science of using correct movement patterns and correct lengths of time spent moving as soon as possible after diagnosing a problem to shorten and improve healing rates.”
Before instituting a rehabilitation plan, however, have your veterinarian perform a complete lameness exam so you have an accurate diagnosis of the problem.
Rehabilitation protocols are horse-specific, but as you work through the first phase of your rehab plan, Schils says to:
- See how “straight” the horse is when walking away from and toward you;
- Look to see if the hind hooves fall into the tracks of the front hooves;
- Observe if both hind and front legs are striding with equal length;
- Ask the horse to take longer and shorter strides and see how he bends in the fore- and hind-limb joints, noting if he loses straightness during these changes in stride length; and
- Discontinue lateral bending exercises in the early stages of rehabilitation. Keep the horse as straight as possible to encourage correct joint alignment and to re-establish correct weight-bearing on the limbs. Then reintroduce correct bending gradually as rehab progresses.
Schils stresses the importance of keeping expectations for the outcome of rehabilitation reasonable, based on the degree of arthritis and the rider or trainer’s skill.
Q: Are horses with arthritis simply not going to improve? Is it really just about managing pain?
Yes. As unpleasant as this answer might be, and despite decades of research in this field in humans and animals, a cure for OA (i.e., reversal of the disease process) remains elusive. Pain control is a key component of managing arthritic horses, which you and your veterinarian can address both pharmaceutically and with complementary and alternative therapies.
“Unfortunately, factors outside the joint environment also impact a horse’s condition, such as the overall health of the animal, endocrine status, rules governing drug usage and withdrawal times in competition, and even owner expectations and financial commitment,” says Contino.

Written by:
Stacey Oke, DVM, MSc
Related Articles
Stay on top of the most recent Horse Health news with















